Your donation will support the student journalists of West High School. Your contribution will allow us to purchase Scholarship Yearbooks, newsroom equipment and cover our annual website hosting costs.
Emmie Boylan: living with spina bifida
English teacher John Boylan’s daughter, Emmie Boylan, has spina bifida, a life-changing condition that affects her mobility and communication.
December 9, 2019
The diagnosis
In December of 2014, English teacher John Boylan and his wife, Sarah Boylan, went to the University of Iowa Children’s Hospital for their daughter, Emilia “Emmie” Boylan’s, 20-week ultrasound. John had taken the morning off of work for what he thought would be a quick, exciting appointment.
It started like most other 20 week ultrasounds. The doctor was able to determine the sex, but John and Sarah said they wanted it to be a surprise. Right after they told the doctor, she noticed something out of the ordinary on the ultrasound.
“The ultrasound [doctor] got really quiet and stopped talking,” John said. “It didn’t feel super celebratory. Usually, it’s one of those things where you go in and they clear you and then you come back in, in however many more weeks. [Instead,] she was like, ‘I think you guys need to go see this high-risk team.’ But she wouldn’t tell us why. I think I was just totally numb to it …. I just got in my car and drove myself 50 minutes to work.”
At the appointment with the high-risk team a few weeks later, they were told that Emmie had spina bifida myelomeningocele (MMC), a neural tube defect where the spine and spinal cord do not form properly. In healthy infants, the neural tube, comprised of the spinal cord and the brain, closes within the first 28 days of pregnancy. As it closes, it acts as a zipper, and ‘zips’ down.
With MMC, the zipper stops partway down the back, leaving a hole that stretches the rest of the way down. Where the hole stops determines how many nerves it affects, and consequently how severe of a case it is. Because of how far down on Emmie’s back the hole was, the doctors assumed she would have a mild case.
“They told us a lot of spina bifida kids live totally normal lives other than they struggle to walk a little bit,” John said. “Based on where her defect was, she would probably be able to walk with braces. With therapy, she might be able to walk unassisted or with a walker or crutches.”
That was our initial diagnosis. [That] she has this neural tube defect, but she’ll live a very normal life, which has not been very true.
— John Boylan
“That was our initial diagnosis,” John said. “[That] she has this neural tube defect, but she’ll live a very normal life, which has not been very true.”
Infographic by Gwen Watson
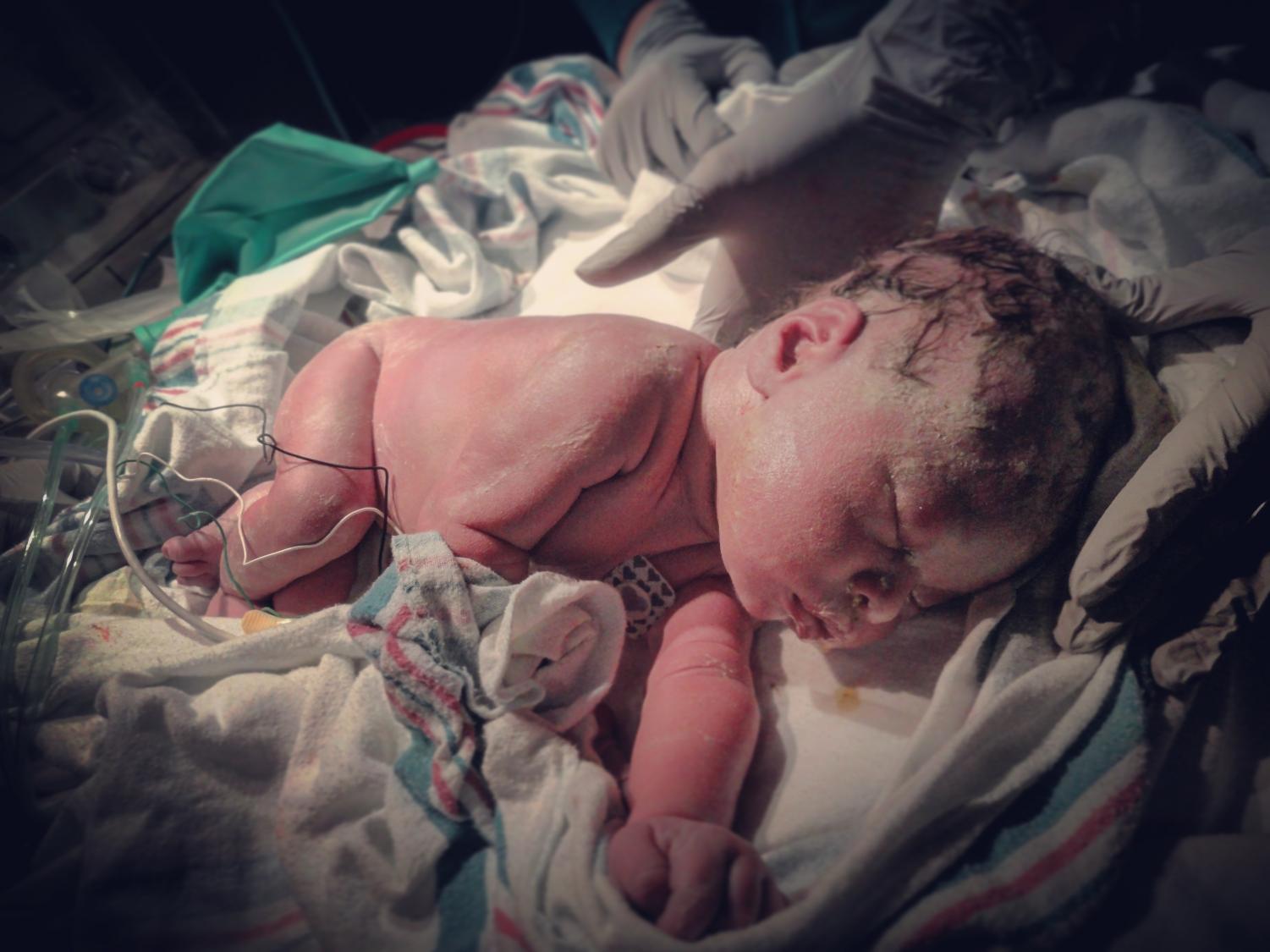
Newborn Emilia “Emmie” Boylan at the University of Iowa Children’s Hospital right after her birth.
The birth
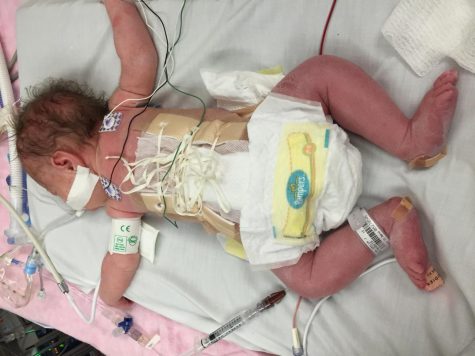
Emilia “Emmie” Boylan after the surgery to close up her back.
Emilia “Emmie” Jane Boylan was born on April 23, 2015. The next day, she had the hole in her back surgically closed up. A week later, the doctors put a valve in her brain to drain the cerebrospinal fluid, or fluid of the brain and spinal cord. Cerebrospinal fluid normally cycles through the neural tube, but with spina bifida, it cannot cycle properly. When the hole is closed up, there is nowhere for the fluid to go so it builds up in the brain. Having fluid in the brain is known as hydrocephalus, and it is a common symptom of spina bifida. Leaving hydrocephalus untreated can lead to nausea, poor balance, seizures or even death. Hydrocephalus needs to be constantly treated with a shunt or a valve.
The valve failed the next week, so Emmie had to have a shunt put in. The shunt is composed of a tube that is inserted into her brain cavity and a machine run by a magnet in her brain. The tube connects to her stomach and drains the fluid so it can be processed and expelled.
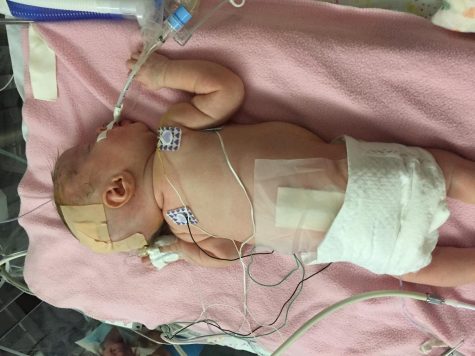
Emilia “Emmie” Boylan at the University of Iowa Children’s Hospital for her first shunt surgery.
Emmie spent a total of one month in the neonatal intensive care unit (NICU) after her birth. When she was born, she failed the Apgar score, which is a series of tests to check infants’ health. She didn’t open her eyes until she was three or four weeks old.
“I remember thinking that was weird,” John said. “But I’m medically illiterate so I knew none of this. My wife is a nurse and she knew immediately like, ‘Oh, my daughter failed the Apgar tests’ …. And I was like, ‘Oh well she just had these big surgeries and so she’s just coming out of sedation. That’s why she hasn’t opened her eyes, or that’s why she’s tired or that’s why she doesn’t squeeze my hand.’”
Infographic by Gwen Watson
The doctors do not know why her case is as severe as it is. One of the biggest realizations came when Emmie was around seven months old when John and Sarah took her to see a neurologist.
“[He] had done a brain scan,” John said. “And we’re like, ‘Well it’s weird she’s not doing any of these milestones that we assumed she’d be able to do.’ He’s like ‘Well obviously not, she has brain hemisphere interdigitation,’ and we’re like, ‘Wait, what, what does that mean?’ And he showed us the scan. I’m sure even in like biology class you’ve seen the two brain hemispheres … Hers is just a big clump and there’s these jagged spaces and there’s not a division of hemispheres.”
Brain hemisphere interdigitation, also known as gyri interdigitation, is when the two hemispheres of the brain are not fully separated. Interdigitation refers to the shape fingers make when linked together. While interdigitation is very rare, it is commonly found with Chiari II malformation. Chiari II malformation occurs when the brainstem and the cerebellum protrude into where the spine connects to the skull. This leads to problems with balance, speaking and breathing.
I would say it took me probably six to eight months to really realize like, ‘Oh, she’s gonna live a very different life than I had imagined she would live.’
— John Boylan
Through the diagnosis of Emmie’s brain hemisphere interdigitation, it became apparent that she would be greatly affected by MMC.
“I would say it took me probably six to eight months to really realize like, ‘Oh, she’s gonna live a very different life than I had imagined she would live,’” John said. “… In some ways it was clarifying because it’s easy to second guess yourself and be like ‘What am I not doing right,’ so to say, like, ‘Oh, you can be trying to do everything right and she might not make progress because her brain [is] not functional in a lot of ways,’ but it’s also kind of hard because that means that you have to kind of accept that it’s not.”
“I think the hardest part is that it’s so far beyond your control. And I never liked not being in control, but if there’s one thing I wish I could control, it’s my daughter’s health, the thing that I care most about,” John said.
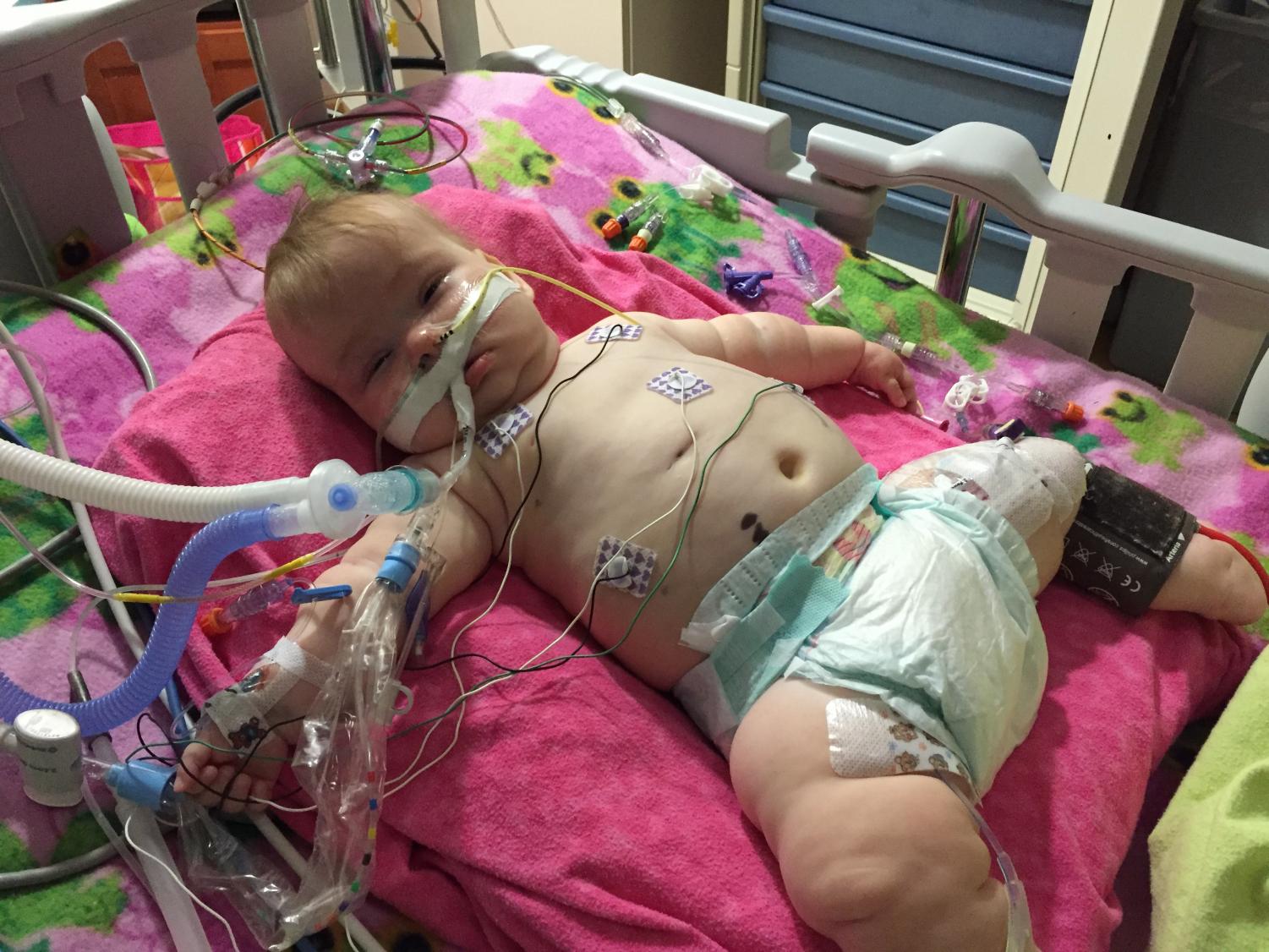
Emilia “Emmie” Boylan after her ventriculostomy surgery around Thanksgiving of 2015.
The brain bleed
Just as they were figuring out the diagnosis was different than they had expected, around Thanksgiving of 2015, Emmie’s shunt for her hydrocephalus failed. It is not uncommon for shunts to fail; in fact, around half of shunts fail within the first two years of being implanted. However, Emmie’s surgery to get the shunt fixed led to a brain bleed. Emmie had a ventriculostomy to drain the blood from her brain. A ventriculostomy involves opening up a ventricle of the brain and placing a shunt in to drain.
All of the blood needed to drain for her to survive and it could take multiple weeks. The Boylans knew the risks of brain bleeds, so they requested to meet with a palliative, or end of life, care team. Sarah had been working on a palliative floor at that time and had seen a lot of patients have to make the same decision. Some families had had invasive surgeries performed even though the patient had no chance of recovery.
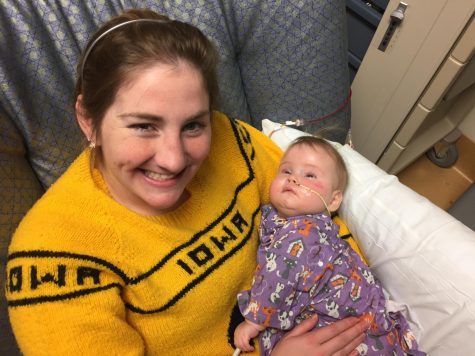
Sarah Boylan and Emilia “Emmie” Boylan recovering from the ventriculostomy surgery.
“We talked a lot about whether we were going to proceed with [the surgery] or let her pass more peacefully without another surgery,” John said. “My grandpa had also died a couple years prior after falling and having a head bleed, and when my wife told my family [that] she didn’t think they should make him go through this intense surgery. My family didn’t listen to her and my grandpa ended up suffering quite a bit and dying a pretty undignified death, which haunts my mom still since Sarah had warned about it. We just didn’t want that for Emmie.”
They decided to go through with the surgery. She had too much of her life ahead of her and enough of a chance to survive. They also learned that she would not be able to pass peacefully.
“If we didn’t proceed, she was going to have a pretty miserable death because she had these quickly increasing brain pressures and she would have trouble breathing and spike a fever and all kinds of stuff. It’s not like she would have been able to die peacefully in her sleep, and I don’t think I could be witness [to] that kind of suffering and know I hadn’t given her a chance,” John said.
The brain bleed took around a month to drain but she recovered fully. During that time, West High was completely supportive of the Boylans.
It was my first year at West so I had no sick or personal days built up, but when I told Molly Abraham the situation, she supported me completely and told me not to worry about anything at school.
— John Boylan
“It was my first year at West so I had no sick or personal days built up, but when I told Molly Abraham the situation, she supported me completely and told me not to worry about anything at school,” John said. “The English department made care packages and some of the teachers came to the hospital to visit us. I remember Jeff Finn and Katy Nahra and I think Peggy Dolson maybe, she’s at Liberty now, ended up coming on a really horrible day when I was completely broken and they managed to support me without intruding, which is a really hard balance to strike.”
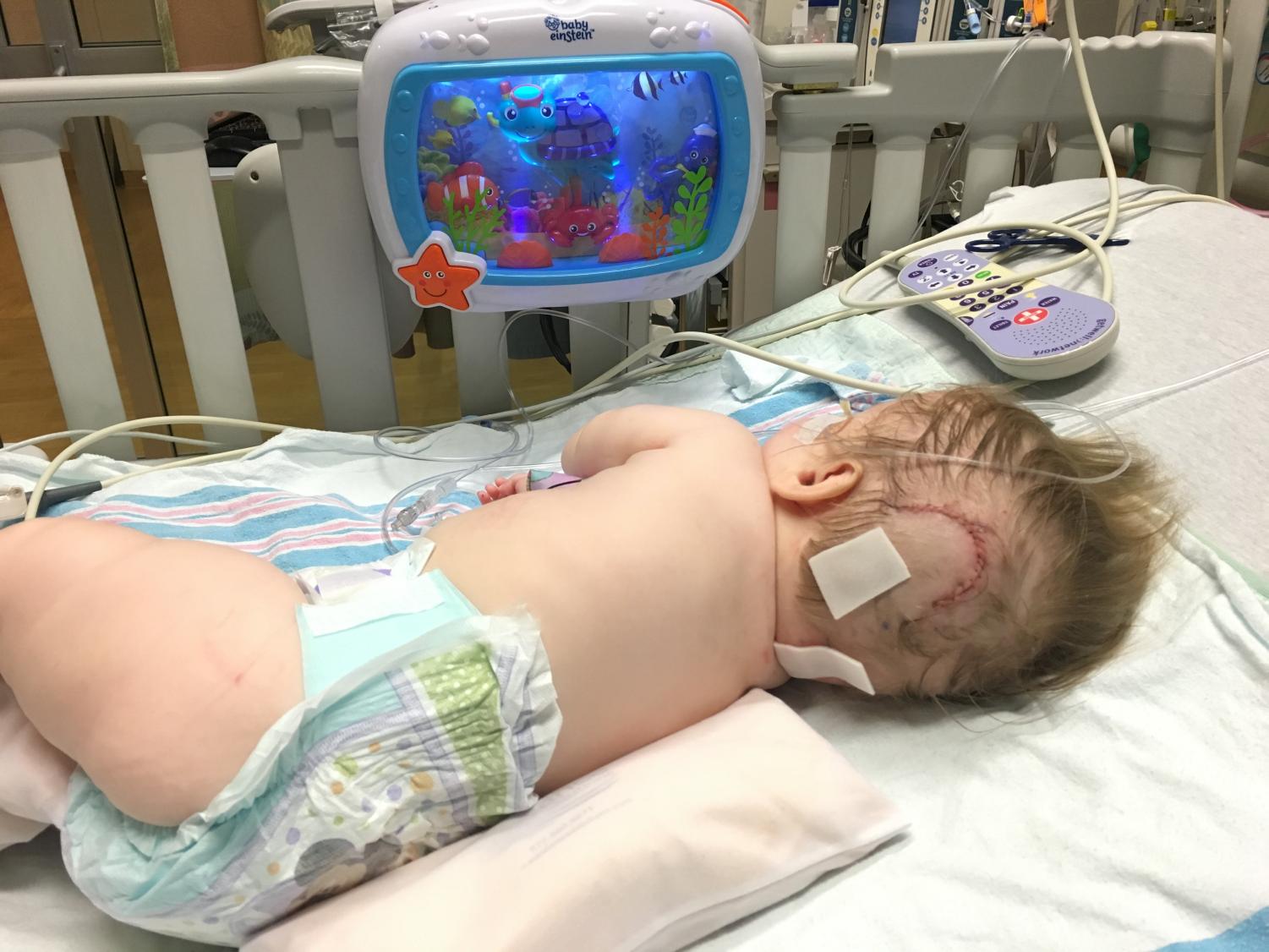
Emilia “Emmie” Boylan after the surgery for her cyst at Lurie Children’s Hospital in Chicago.
Lurie Hospital
Although Emmie had recovered from the brain bleed, it wasn’t over yet. The scans from the brain bleed showed a cyst that had formed in Emmie’s brain where her cerebellum was supposed to be. However, the neurosurgeons did not notice the cyst until a few months later.
“We were not very confident with the doctors here,” John said. “They told us ‘Oh the cyst was on the scans six months ago.’ We were like, ‘Why did you not tell us about that then?’ They’re like, ‘We didn’t really notice it.’ ‘You noticed it now how did you not notice it then?’ They’re like ‘Well we weren’t really looking for it.’”
The cyst and the brain bleed made it hard for the Boylans to trust the U of I Children’s Hospital. They moved Emmie’s care to Lurie Children’s Hospital in Chicago, where there is a spina bifida clinic. The clinic made it more efficient. Even though they had to drive to Chicago, they were able to see all of their specialists in one day. When they were with the U of I, they had to take Emmie to appointments three or four times a week.
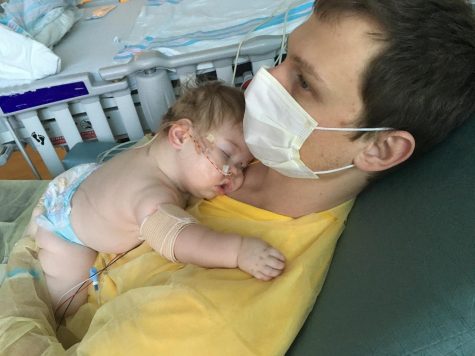
John Boylan holding Emilia “Emmie” Boylan during the recovery for Emmie’s cyst surgery.
John was able to go along even though he still did not have any sick days to take. The English department was just as helpful with the cyst. They made substitute plans, lesson plans and graded his papers. He also received gifts and cash from the West High staff that they were able to use to pay for travel and lodging in Chicago.
“These are all people I now have deep professional relationships with, but back then, we were just a few months into my career at West,” John said. “It was remarkable. Every day at the hospitals, we would see parents trade off who was staying with their kid while the other had to leave for work, and for my wife and I to both be able to be there together. I don’t know how to quantify how much that meant to me.”
Every day at the hospitals, we would see parents trade off who was staying with their kid while the other had to leave for work, and for my wife and I to both be able to be there together. I don’t know how to quantify how much that meant to me.
— John Boylan
Emmie had the surgery for her cyst at Lurie and a follow up due to a blockage. The doctors drained the cyst with a shunt that connected to her existing shunt in a y-shape. After two years they switched her back to the U of I. They knew if there was ever an emergency they would not be able to fly all the way to Chicago.
While the Boylans have had complications with hospitals as a whole, they have received a great deal of help from certain nurses who have spent a lot of time with Emmie.
“The things that have been most helpful have been individual nurses who have made us feel like they believe in Emmie as much as we do, or they are as loving towards her as we are,” John said. “I think the biggest thing that doctors can do is be transparent, be honest about things and give you time, because it’s really hard when she’s your everything and the doctor’s like ‘Here’s the five minutes I can give you.’”

A photo from Emilia “Emmie” Boylan’s invitation to her first birthday party.
Symptoms

Emilia “Emmie” Boylan sitting in her adaptive chair while wearing sunglasses.
Aside from having a severe case of MMC, Emmie also has some symptoms that are not linked to spina bifida. Emmie has minor hearing loss, so she has had tubes put in twice and has hearing aids. In addition, she has hypotonia, or low muscle tone, to a degree where she almost always uses an adaptive chair. Her hypotonia also means that she has sleep apnea. Sleep apnea is a condition where her airway closes off when she is sleeping. She’s not strong enough to keep it open when asleep.
“She reacts the way you or I would if we tried to hold our breath for as long as we could and then do this wake up kind of panic. So in the middle of the night [sleep apnea] keeps her from sleeping,” John said.
The Chiari II malformation and hypotonia both affect Emmie’s coordination. She has little fine motor control so she has a hard time playing with toys and she cannot feed herself. Her hypotonia also means that she can only eat soft foods like pudding, milk and soft fruits.
“Either my wife or I or someone else basically always has to be with her, otherwise she just lays there,” John said. “One of us is always trying to position her body in tummy time so she can swipe and play with the toy, or trying to help her balance herself as she sits up or holding her a certain way so that she can reach to turn the pages as we’re reading books.”
Infographic by Gwen Watson
To help improve her motor control she has physical therapy and occupational therapy. Occupational therapy helps patients live their fullest life. They work on cognitive, physical, sensory and motor skills. Occupational therapy is more common among adults because children do not have jobs, but occupational therapy helps kids with school and daily activities.

She has a wide range of other therapies to help as well including feeding therapy, which teaches kids to eat and helps them with their eating schedule; music therapy, which uses music to help mental health; and aquatic therapy, which is a form of physical therapy where exercises are performed in the water. Finally, Emmie has equine therapy, or horse therapy, where she gets strapped into a horse saddle and the horse walks around to help improve her balance.
“I always think of it as like when I played football, you knew you were strong if you could lift while you were on a medicine ball, because it was like a stability kind of thing,” John said. “So the horse therapy like requires her to … hold her balance and hold her strength that way.”
Emmie is also nonverbal, which is not commonly associated with spina bifida. She has two speech-language pathologists (SLP), one at Borlaug Elementary, where she goes to pre-kindergarten in the afternoons, and one at ChildServe, an organization that helps with the rehabilitation and care of children.
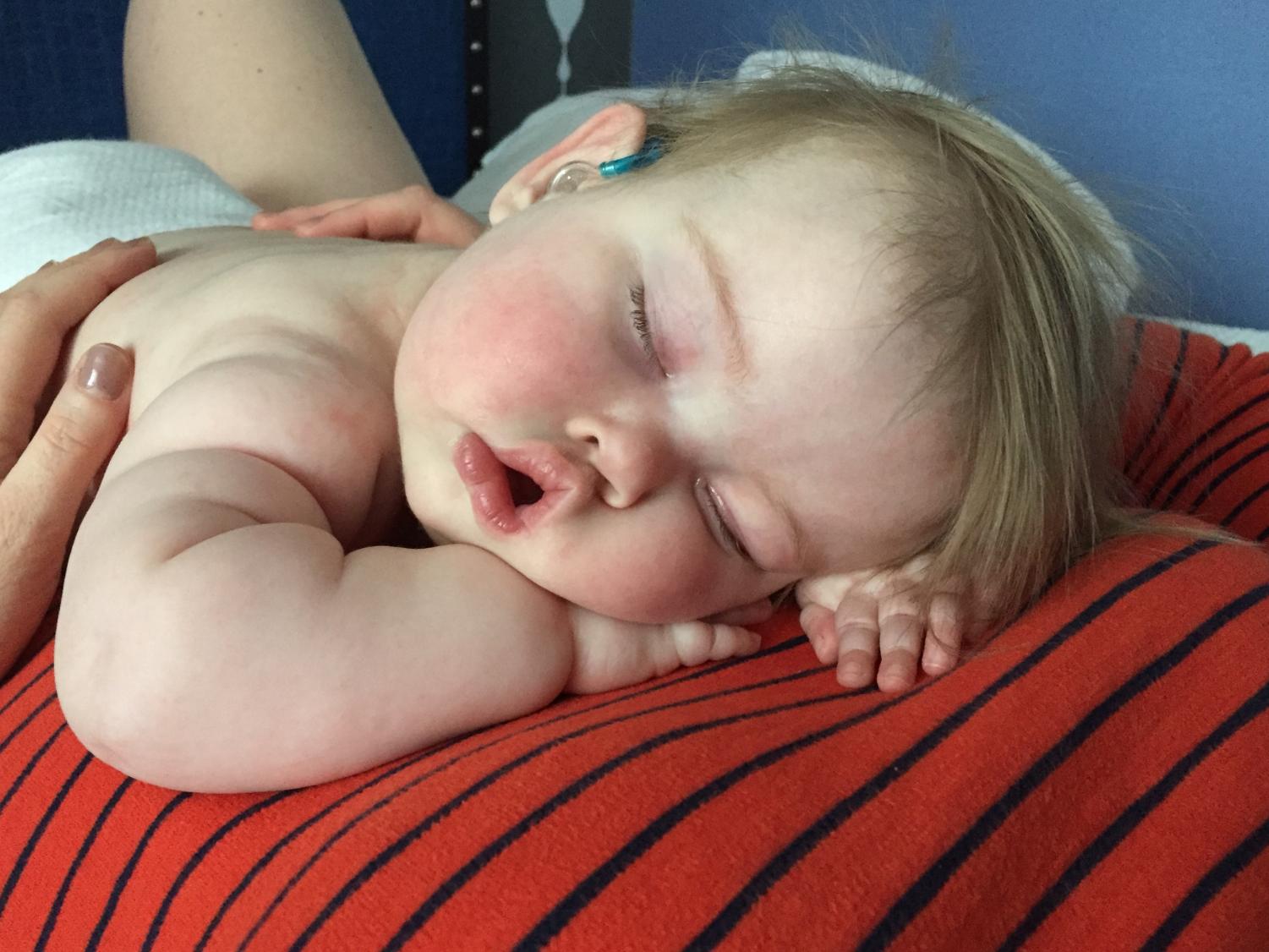
Sarah Boylan holding her daughter, Emilia “Emmie” Boylan, as she sleeps.
Communication
The Boylans have used multiple different technologies to help Emmie communicate. The first one they used was just a large trifold with velcro pictures of different objects. They would hold up two photos and ask Emmie which one she wanted. To choose, she looked at the one she wanted. Over the years, Emmie has gotten new devices, but all of them had their drawbacks.
However, at the beginning of the school year, the Boylans got a Tobii Dynavox 13. The device has icons that correlate with certain words and phrases. It uses eye-tracking software to determine what Emmie wants to say and then verbalizes it for her.
“If she looks at one that says ‘I am happy’ it will say, ‘I am happy.’ She can look at all kinds of stuff and it does the work of flipping through the flipbook together,” John said. “So she says, ‘I want to do an activity [or] I want to read a book.’ And then it takes you to another page.”
The device is known as an Alternative-Augmentative Communication (AAC) device. AAC is any form of communication that does not involve speaking.
“We all use symbols to communicate our thoughts. Most of us use words as those symbols, and we speak them so that others hear our message. Sometimes, we have students who need other supports to represent their thoughts and communicate with others. Alternative-Augmentative Communication is a way for those students and people to utilize a different system of symbols to communicate,” said Ali McCue, Emmie’s speech-language pathologist at Weber Elementary during the 2018-2019 school year.
McCue worked with Emmie on increasing how much language she uses. Emmie was very good at asking for things but she often did it through crying or laughing, not using a device. Their focus was to increase how much she used the device. However, when McCue was Emmie’s speech-language pathologist, she did not have the eye gaze device yet.
“Emmie had a ‘light tech’ system last year. It was a binder with a hole cut in the middle. There were pictures around the outside of the hole. Emmie had to use her eyes to look at the symbol she wanted to use. We worked on increasing her speed at finding words, learning new words, and using words as much as she could.” McCue said.
The Boylans originally had the Toby Dynavox 13 for just a trial period, but as of the week of Nov 17, they officially own one. Their goal now is to help her learn what the different icons mean and where they are on the device.
“All of our communication with her now has to happen through the pod,” John said. “So I ask her questions but then I say back what I’m thinking, or if we’re reading the characters in the book, I would say, ‘Oh, I think the monster feels sad, Emmie, because he doesn’t have any friends.’ So then I would find the monster button and then find the sad button and you basically have to narrate everything.”
Teaching Emmie where to find what she wants to say through the device is known as modeling. Modeling is used by everyone when they are learning to speak. Parents or other people show babies the right way to use language by speaking.
“We do the same for our students whose language learning is delayed. For students with AAC, we use their symbol systems to show them how to communicate with it. We model what the symbols mean, where they are in the device, and how a student might use it.” McCue said.
While the Boylans don’t know how much letter recognition she has, Emmie loves to read books. Some of Emmie’s favorite books include “Pete the Cat and the Four Groovy Buttons” and “Brown Bear Brown Bear”. She has these memorized to the point where she knows what happens on each page. The Dynavox also helps her read books with her parents.
“She could theoretically, go to Brown Bear Brown Bear and click like ‘What do you see?’ with her eyes, so I could say, ‘Brown bear brown bear,’ and then she would say, ‘What do you see?’ And then I would read back [to her],” John said.
The device is completely customizable so the order of the icons can be moved around. Currently, they are alphabetical, but they can make a hot button page for the icons Emmie uses the most. She also has an About Me page that she can use at school. The eye gaze device has improved her autonomy drastically.
“Emmie’s progress has been really amazing,” McCue said. “From what I saw this summer, Emmie’s independence, autonomy and quality of what she could say drastically increased with her high-tech system. She went from barely meeting her goal to almost meeting it in a few weeks. That was the power of finding a system that was more in line with her needs and a team that is constantly problem-solving to help find the best for her. I can’t wait to see how much she’s grown when she comes to Kindergarten.”


